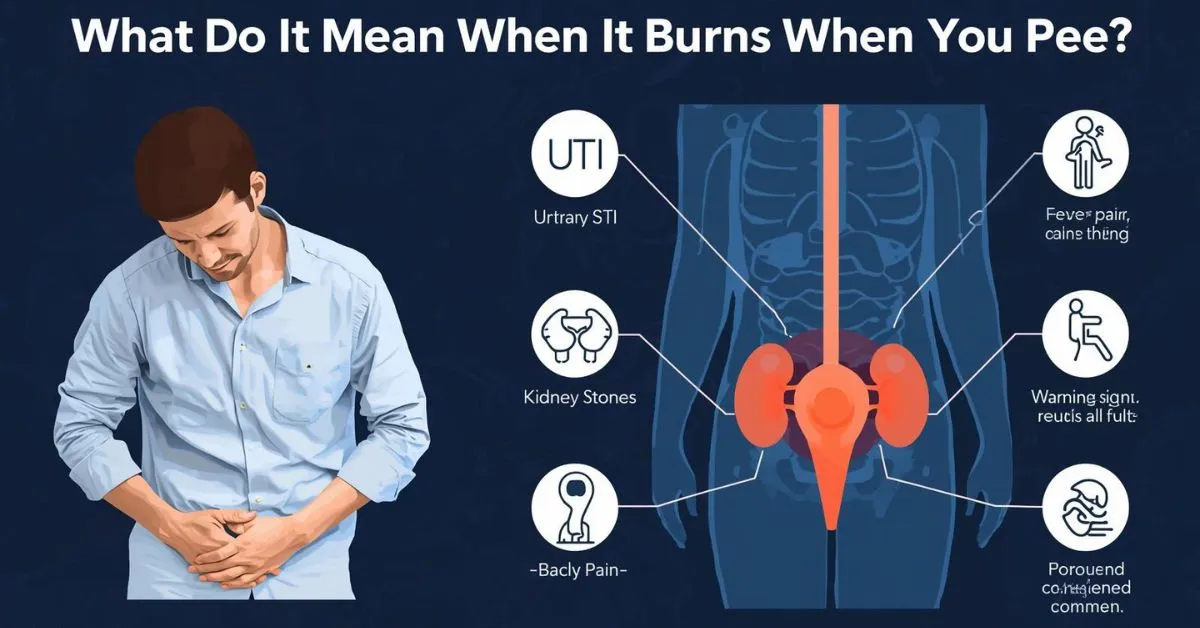
Burning when you pee usually means something in the urinary tract or nearby genital tissue is irritated, inflamed, or infected. A urinary tract infection is common, but it is not the only cause.
Burning can also happen with STIs, vaginitis, yeast infections, prostatitis, kidney stones, genital herpes, menopause-related dryness, or irritation from soaps and other products.
The medical term for this symptom is dysuria. That word does not name a disease by itself. It simply means pain, burning, or discomfort with urination, and the cause has to be worked out from the full pattern of symptoms.
What to Do Right Now
Get medical care promptly if the burning does not go away, or if you also have fever, chills, back or side pain, nausea, vomiting, cloudy urine, bad-smelling urine, blood in your urine, discharge, or genital sores. Painful urination in pregnancy should also be reported to a clinician.
You should also get checked sooner rather than later if you are male, pregnant, a child, older or frail, have diabetes, use a catheter, or keep getting this symptom repeatedly. Those groups can have more complicated urinary problems or need faster evaluation.
Why It Burns When You Pee
In simple terms, burning happens when urine passes across tissue that is inflamed, infected, irritated, or injured.
Sometimes the problem is inside the urinary tract, such as the bladder, urethra, or kidneys. Other times the problem is outside the urinary tract, such as irritated vulvar or vaginal tissue that stings when urine touches it.
That is why the same symptom can come from very different causes. Burning with urgency and frequent urination points in one direction. Burning with discharge, sores, or itching points in another.
The Most Common Causes
Urinary tract infection or cystitis
A UTI is one of the most common reasons it burns when you pee. Typical clues include a strong urge to urinate, going more often, passing small amounts, cloudy urine, blood in the urine, pelvic discomfort, and sometimes a low fever. Women get UTIs more often than men, in part because the urethra is shorter.
If a bladder infection is not treated or does not clear, it can move upward and become a kidney infection, which is more serious.
STI-related urethritis
Burning when you pee can also come from urethritis, which means inflammation of the urethra. Sexually transmitted infections such as chlamydia and gonorrhea are common infectious causes.
A discharge from the penis or vagina, bleeding between periods, testicular pain, or a recent sexual exposure can make this cause more likely.
One reason people misread this symptom is that STI symptoms can be mild or absent, especially in women. Gonorrhea, for example, may be mistaken for a bladder or vaginal infection when symptoms do appear.
Vaginitis, bacterial vaginosis, or yeast infection
If you have a vagina, burning may come from vaginitis or other vaginal conditions rather than the bladder itself. Vaginitis can cause discharge, itching, irritation, painful sex, spotting, and painful urination.
Bacterial vaginosis can also cause a fishy odor and burning during urination, while a yeast infection often causes itching, vulvar soreness, and a burning feeling during urination or sex.
This is important because urine may sting when it touches inflamed tissue around the vaginal opening, even if the urinary tract is not the main problem.
Genital herpes
Genital herpes can cause pain when you pee, especially if urine passes over open sores or blisters. Tingling, burning, itching around the genitals, unusual discharge, and visible blisters or sores make herpes more likely than a simple UTI.
Prostatitis
In people with a prostate, burning during urination can be linked to prostatitis, which is inflammation of the prostate. Other clues include difficulty peeing, needing to pee more often, pain in the penis, scrotum, testicles, or bottom, pain with ejaculation, and sometimes a high temperature.
Kidney stones
A kidney stone can also make urination painful. Stones are more likely if the burning comes with sharp pain in the back, side, lower abdomen, or groin, blood in the urine, nausea, vomiting, or difficulty passing urine.
Kidney infection
A kidney infection is more urgent than a routine bladder infection. It can cause fever, chills, nausea, vomiting, back or side pain, frequent urination, and cloudy, dark, bloody, or foul-smelling urine.
Menopause-related dryness and urinary irritation
After menopause, lower estrogen can lead to genitourinary syndrome of menopause, which can cause vaginal dryness, burning, itching, frequent or urgent urination, burning during urination, and more frequent urinary tract infections.
This is a commonly missed reason for persistent burning, especially when infection tests keep coming back negative.
Irritants, medicines, trauma, and less obvious causes
Not every case is an infection. Reliable clinical references also list soaps, perfumes, personal care products, some medicines, local trauma, dermatologic irritation, urethral narrowing, foreign bodies, and interstitial cystitis or painful bladder syndrome as possible causes of dysuria.
A Quick Symptom Pattern Guide
This table can help you think more clearly about what might be going on. It cannot confirm a diagnosis, but it does show why the surrounding symptoms matter.
| Symptom pattern | More likely causes |
|---|---|
| Burning + urgency + frequent urination + cloudy urine | UTI / cystitis |
| Burning + discharge + recent sexual exposure | Urethritis / STI |
| Burning + itching + odor or unusual discharge | Vaginitis / bacterial vaginosis / yeast infection |
| Burning + blisters or sores | Genital herpes |
| Burning + trouble peeing + pelvic or testicular pain | Prostatitis |
| Burning + sharp side, back, groin, or lower belly pain + blood in urine | Kidney stone |
| Burning + fever + chills + nausea + back or side pain | Kidney infection |
| Burning + repeated negative infection tests + bladder pressure or pelvic pain | Painful bladder syndrome / interstitial cystitis |
| Burning after menopause + dryness + recurrent irritation | Genitourinary syndrome of menopause |
These symptom patterns reflect the cause-and-symptom groupings described by Mayo Clinic, NHS, CDC, NIDDK, and AAFP.
Burning When You Pee but It Isn’t a UTI
This is one of the biggest reader pain points, and it matters because a lot of people assume “burning = UTI.”
That shortcut is often wrong. If the urine test is negative, clinicians may think about urethritis, vaginitis, yeast infection, herpes, menopause-related changes, irritants, medication side effects, local trauma, urethral stricture, or interstitial cystitis/bladder pain syndrome.
A related clue many articles skip is timing. Cleveland Clinic notes that pain at the start of urination often points toward the urethra, while pain after urination can suggest a bladder or prostate problem. That is not enough to diagnose the cause on its own, but it can be a useful clue.
What Other Symptoms Can Tell You
The burning itself matters, but the companions matter more:
- Frequent urination, urgency, cloudy urine, pelvic pressure: more suggestive of a bladder infection.
- Discharge, bleeding between periods, recent sexual exposure: raises suspicion for urethritis or an STI.
- Itching, odor, vaginal soreness, painful sex: points more toward vaginitis, bacterial vaginosis, or yeast infection.
- Blisters or sores: makes herpes more likely.
- Back or side pain, nausea, vomiting, fever, chills: raises concern for stones or kidney infection.
- Trouble starting urination, weak flow, pelvic or testicular pain: can fit prostatitis or another prostate-related problem.
How Doctors Find the Cause
Clinicians usually start with your symptom history and a urine test. A urinalysis can check for blood and white blood cells, and a urine culture can identify bacteria and help determine whether antibiotics are appropriate.
If the pattern suggests an STI, testing may also include urine testing or swabs. If stones, structural problems, or complicated infection are suspected, imaging or further evaluation may be needed.
Treatment Depends on the Cause
There is no single best treatment for “burning when you pee” because treatment depends on the reason it is happening. Cleveland Clinic notes that treatment can range from antibiotics and avoiding irritants to treatment for the underlying condition.
In practice, that often means:
- UTIs and some bacterial infections: antibiotics may be used.
- STIs: treatment depends on the infection and should be guided by a clinician.
- Yeast infection: antifungal treatment may be used, but Mayo Clinic advises getting checked if symptoms are new, uncertain, or not improving.
- Irritation from products: removing the trigger matters. Soaps, perfumes, deodorant sprays, and other genital-area products can irritate the urethra or surrounding tissue.
- Menopause-related dryness: treatment may be available, so it is worth discussing rather than silently putting up with it.
What You Can Do While Waiting to Be Seen
If you think the cause may be urinary irritation or a simple bladder infection, general self-care often includes drinking fluids and avoiding harsh soaps, deodorant sprays, and scented personal care products around the genital area. Mayo Clinic also recommends not delaying urination when you feel the urge.
But self-care should not replace medical evaluation when symptoms are persistent, severe, or paired with warning signs. A kidney infection, kidney stone, STI, or prostate problem can all start with the same “it burns when I pee” complaint.
What Most Articles Miss About This Topic
Most articles stop at “it’s probably a UTI,” but the more useful question is where the burning is coming from. It may come from the bladder, urethra, kidney, prostate, vagina, vulva, or skin around the opening of the urethra. That is why the symptom by itself does not tell the whole story.
Another thing many pages miss is that mild STI symptoms can look like a UTI. Gonorrhea and chlamydia can cause burning when you pee, and some people have only subtle symptoms or none at all.
A third blind spot is menopause-related urinary burning. When infection tests are negative but the symptom keeps returning, low-estrogen tissue changes may be part of the answer.
FAQ
Is burning when you pee always a UTI?
No. UTIs are common, but painful urination can also be caused by STIs, vaginitis, yeast infections, genital herpes, prostatitis, kidney stones, bladder pain syndrome, menopause-related changes, and irritants such as soaps or perfumes.
Can dehydration make it burn when you pee?
Dehydration is not one of the main diagnosis categories listed by the medical sources above, but concentrated urine may feel more irritating when tissues are already inflamed. Persistent burning still needs proper evaluation rather than guesswork. This is an inference based on the role of irritation and the advice to maintain fluids, not a standalone diagnosis category.
What if it burns when I pee but my urine test is negative?
That can happen. Clinicians may then consider urethritis, vaginitis, yeast infection, herpes, irritants, structural problems, medication effects, painful bladder syndrome, or menopause-related changes.
Why does it burn when I pee after sex?
A post-sex burning sensation can happen if sex caused friction or local irritation, but it can also happen with UTIs, vaginitis, yeast infections, or STIs. If it keeps happening or comes with discharge, odor, sores, fever, or blood in the urine, get checked. This is partly an inference from the documented causes and symptom overlap.
When should I worry?
Worry more if the symptom does not go away, or if you also have fever, flank pain, nausea, vomiting, cloudy or bloody urine, discharge, sores, pregnancy, or difficulty urinating. Those are stronger signals that you should not just wait it out.
Conclusion
If it burns when you pee, the most helpful takeaway is this: it is a symptom, not a diagnosis. A UTI is common, but it is only one of several possible causes.
The safest way to interpret the symptom is to look at the full pattern: frequency, urgency, discharge, odor, itching, sores, blood, flank pain, fever, pregnancy status, and whether the problem is getting worse. If red flags are present, get medical care instead of guessing.
Click Below To Read About:
What Does BTW Mean? Meaning, Examples, and When to Use It
What Does Eminent Domain Mean? Public Use and Compensation
What Does PPF Mean? Finance, Cars, Economics, and Pensions

Hi, I’m Clara Lexis from Meanvia.com. I break down words and expressions so they’re easy to understand and enjoyable to learn. My mission is simple: make language approachable and fun, one word at a time.